
High-altitude illnesses such as acute mountain sickness (AMS), high-altitude pulmonary edema (HAPE), and high-altitude cerebral edema (HACE), can afflict novices as well as the most experienced mountaineers.
HAPE, or high-altitude pulmonary edema, is actually the number 1 killer among these altitude illnesses. HAPE typically begins to affect climbers, riders and mountaineers head abruptly on the second night an individual or team spends above 8,000 feet (or 2,500 meters). Specifically, HAPE is a life-threatening form of non-carcinogenic pulmonary edema (fluid accumulation in the lungs) that occurs in otherwise healthy people at altitudes typically above 2,500 meters or 8,200 ft.
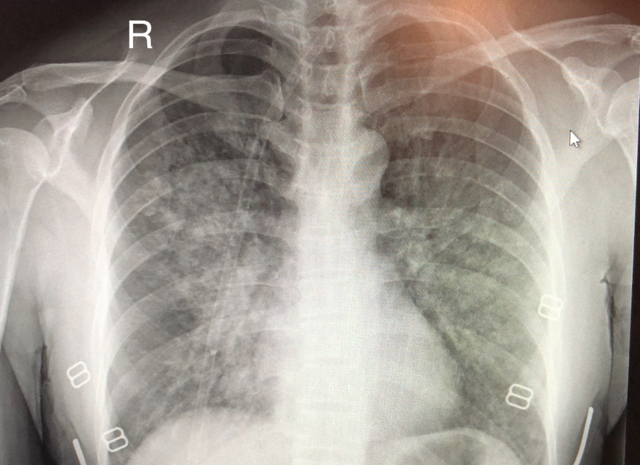
When suffering from HAPE, the arteries in one’s lungs begin to constrict, increasing pulmonary blood pressure. This causes fluid to leak into the air sacs of the lungs, resulting in a gas exchange that ends up reducing the lungs’ ability to absorb oxygen.
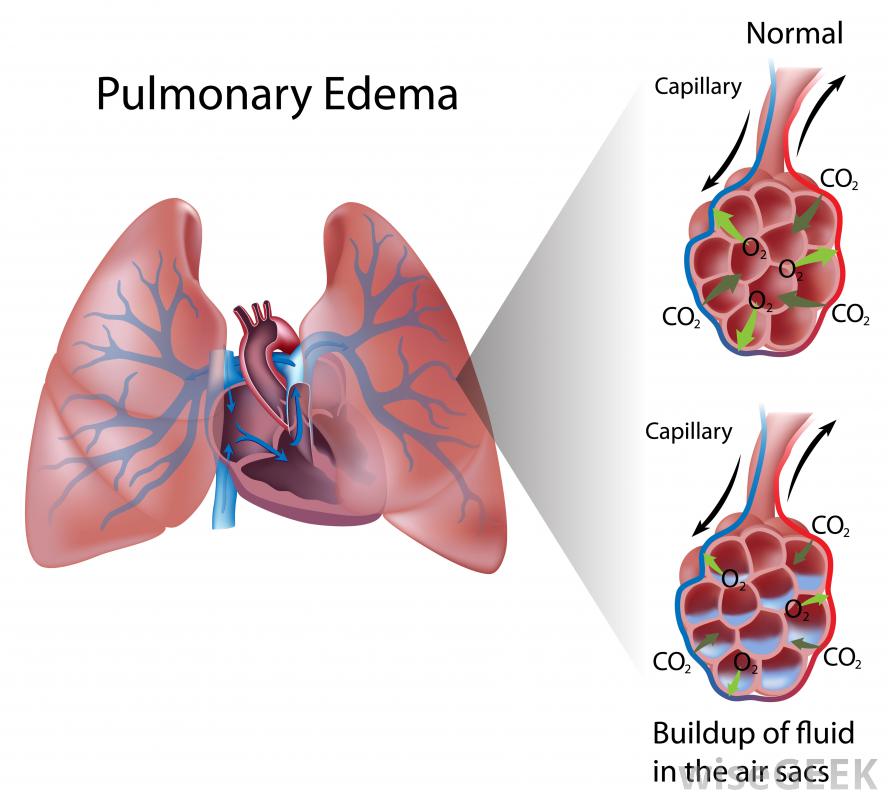
Signs and Symptoms of High Altitude Pulmonary Edema (HAPE)
The Lake Louise Consensus Definition for high-altitude pulmonary edema established widely used criteria for defining HAPE symptoms. Symptoms vary with physiological and symptomatic changes often vary according to the altitude involved. However, the presence of at least two of the following symptoms while recently gaining altitude may allude to the presence of HAPE:
- Shortness of breath, even while at rest
- Cough
- Weakness or decreased exercise performance
- Chest tightness/ congestion
Signs of: (at least two):
- Crackles or wheezing (while breathing) in at least one lung field
- Central blue skin color
- Tachypnea (rapid breathing)
- Tachycardia (rapid heart rate)
Patients often present with decreased exercise performance, shortness of breath at rest, and a dry cough. Because shortness of breath while exercising and cough are common at altitude, HAPE victims are often initially unaware they have it. Heart and breathing rates are elevated. As HAPE progresses, you may hear bubbling lung sounds, commonly known as “rales”. Climbers may also reveal bluish lips and nailbeds (cyanosis), and cough up pink, frothy sputum. In addition, one may have HAPE and HACE concurrently.
Acute mountain sickness and high-altitude cerebral edema may also be present in conjunction with HAPE. However, these symptoms may be subtle or even not present at all. The most reliable sign of HAPE is severe fatigue or exercise intolerance, especially in a climber previously not displaying such symptoms
What Causes HAPE?—The Risk Factors:
At a basic level, HAPE occurs when blood vessels in the lungs constrict as a result of a lack of oxygen, causing fluid to leak into the lungs. This prevents the oxygenation of the blood, which if not recognized and untreated in a timely manner, may become fatal, making it essential to recognize the symptoms of HAPE right away.
At high altitudes, air pressure decreases resulting in “thinner” air—that is, oxygen molecules spread farther apart. We take in less oxygen when breathing at these higher altitudes, resulting in less oxygen being absorbed in the lungs and delivered to the body. A low-oxygen state, whether in ambient air or in the body, is called hypoxia.
Experts warn that exercise at high altitudes may adversely affect those with pre-existing conditions and other health issues when coupled with a variety of environmental and personal factors.
HAPE is observed in a variety of scenarios. In many instances, people residing at lower altitudes who then travel to an altitude above 2,500 meters (8,200 feet), are found to be more commonly susceptible to altitude sickness because their bodies are not acclimatized.
Yet even those who live at higher altitudes could be susceptible to “re-entry HAPE,” a severe presentation of altitude sickness that occurs in persons who normally live at high altitude but who develop pulmonary edema after returning from a stay at low altitude
Risk Factors:
– Sex (males are apparently more susceptible)
-Genetics
-Prior diagnosis of HAPE
-A party’s rate of ascent and/or Cold Exposure
-Peak Ascent, Intensity of Physical Exertion
-Certain underlying medical conditions including, pulmonary hypertension and other predisposing anatomic abnormalities that increase pulmonary blood flow.