
A new study is linking living at altitude to lower rates of COVID-19 infection, great news for our mountain-dwelling readers. The abstract of the study is below:
In the present study, we analyze the epidemiological data of COVID-19 of Tibet and high-altitude regions of Bolivia and Ecuador, and compare to lowland data, to test the hypothesis that high-altitude inhabitants (+2,500 m above sea-level) are less susceptible to develop severe adverse effects in acute SARS-CoV-2 virus infection. Analysis of available epidemiological data suggests that physiological acclimatization/adaptation that counterbalances the hypoxic environment in high-altitude may protect from the severe impact of acute SARS-CoV-2 virus infection. Potential underlying mechanisms such as (i) a compromised half-live of the virus caused by the high-altitude environment, and (ii) a hypoxia-mediated downregulation of angiotensin-converting enzyme 2 (ACE2), which is the main binding target of SARS-CoV-2 virus in the pulmonary epithelium are discussed.
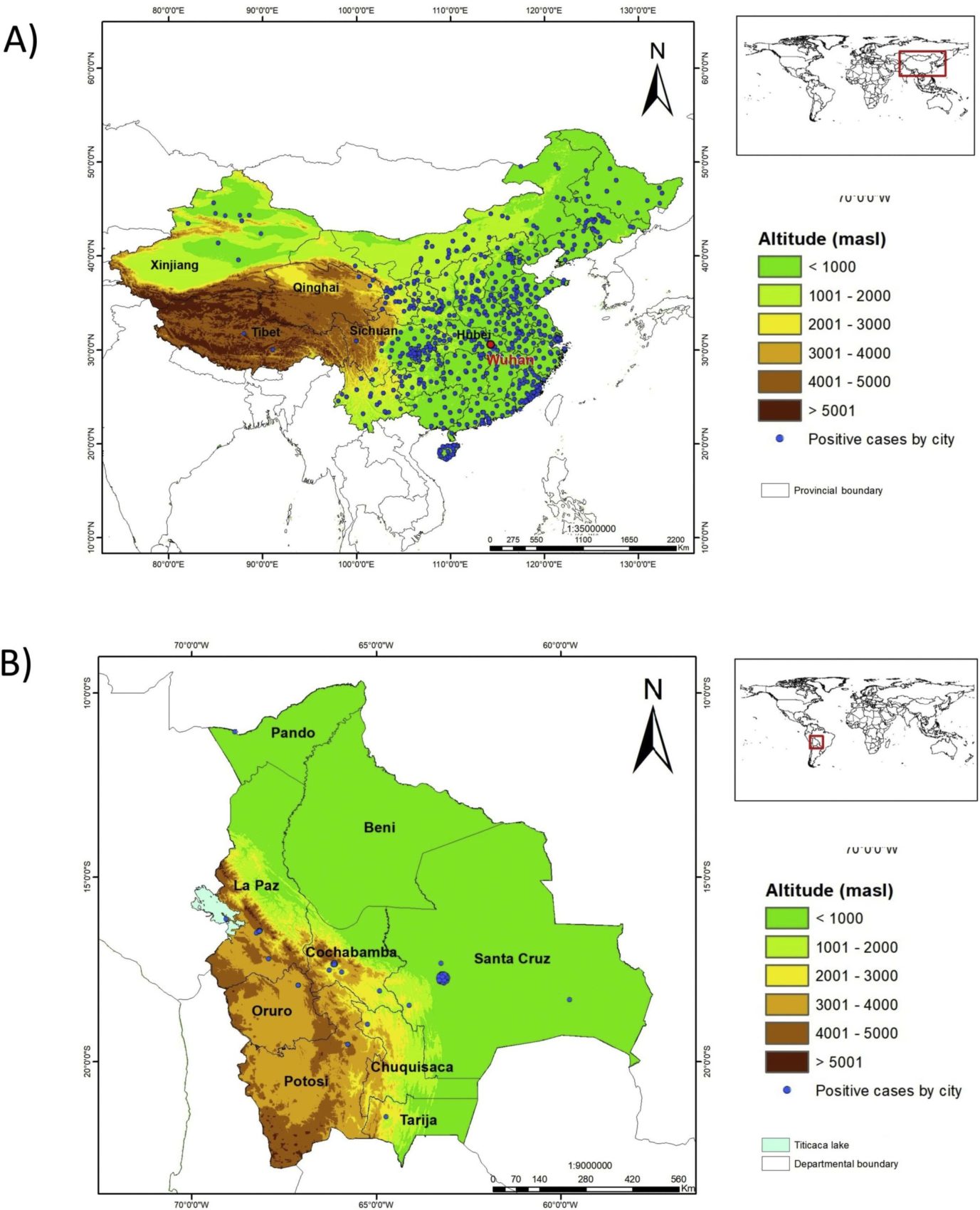
The researchers studied populations at a number of high-altitude areas around the world. On the Tibetan plateau, in China, the impact of COVID-19 on the population of 9-million has been drastically low compared to the rest of China, only 134 cases have been confirmed. In Bolivia, only 410 cases out of the nation’s 8,387 have been confirmed at higher altitudes. In Ecuador, confirmed cases are four times higher in coastal areas compared to higher altitude areas.

In the high-altitude Peruvian city of Cusco, home to 420,000, there has been no new coronavirus related deaths since April 3, even as the disease has claimed more than 4,000 lives nationally. And the infection rate is low, according to the Washington Post. Only 916 of Peru’s 141,000 cases come from the Cusco region, meaning its contagion rate is more than 80 percent below the national average.
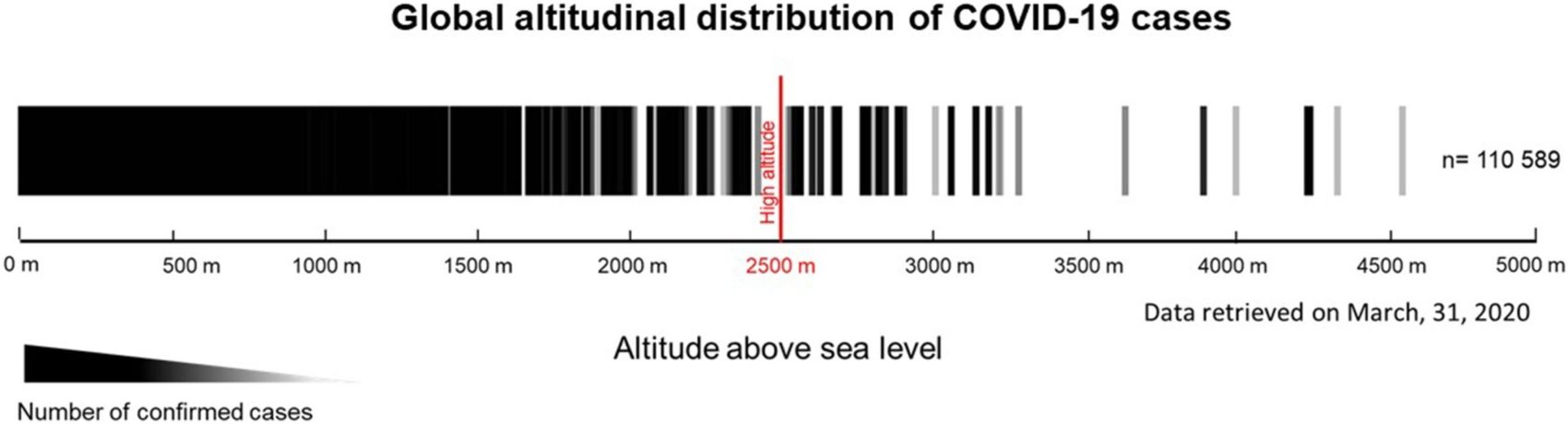
Worldwide, there are approximately 120 towns and cities located over 3,000-meters above sea-level (9,842-feet). Analyzing real-time data, researchers found a distinct decrease in infection rates for populations living above 3,000-meters.
Our epidemiological analysis of the Covid-19 pandemic clearly indicates a decrease of prevalence and impact of SARS-CoV-2 infection in populations living at altitude of above 3,000 masl.
The study concludes there are two factors involved as to why this is the case related to both environmental factors and physiological factors. High-altitude environmental factors, such as temperature, air dryness, and high levels of UV light radiation may all decrease the effectiveness of the virus. Also, due to the lower density of air at altitude, the virus must be smaller and therefore less effective than at sea-level.
It is clear that, all together, these factors may dramatically reduce the “survival” capacity of the virus at high-altitude, and therefore its virulence. Finally, due to the lower density of air and greater distance between molecules at high-altitude, the size of the airborne virus inoculum must be smaller than at sea level.
Secondly, the acclimatization of people living at higher elevations may make them physiologically less susceptible to the virus.
Highland inhabitants may be less susceptible to SARS-CoV-2 virus infection due to physiological acclimatization to hypoxia.
We know that when the virus attacks a person’s lungs it causes hypoxia (oxygen deficiency in the body), similar to being at high-altitude. People living at high-altitude adapt to this and already have a tolerance to hypoxia, potentially helping them fight the virus.
We conclude that the virulence of SARS-CoV-2 is reduced at high-altitude due to the physiological acclimatization of its inhabitants, and due to particular environmental characteristics. Furthermore, additional physiological acclimatization of high-altitude living associated with increased ventilation (Soliz et al., 2005), augmented arterial oxygen transport (Lundby et al., 2007), and higher tissue oxygenation (Kimakova et al., 2017), mainly (but not exclusively) mediated by erythropoietin could be explored for potential therapy (see Soliz et al., 2020, same issue RSPNB) of acute respiratory distress associated with COVID-19.
One thought on “Update: People Living at Altitude May be Less Susceptible to Coronavirus”